kottke.org posts about science

An amazing capture of galaxy Messier 104, aka the Sombrero Galaxy, by the 570-megapixel Dark Energy Camera mounted on a Chilean observatory.
The Sombrero galaxy (Messier 104) is a galactic masterpiece that captivates scientists and astronomy enthusiasts alike. Its intricate system of globular star clusters lends insight into stellar populations, and astronomers are intrigued by the supermassive black hole at its center. Its distinctive visual features and relative brightness make it a favorite among amateur astronomers. The fascinating story of its discovery, involving three esteemed astronomers, has earned it a spot on one of the most important lists of deep sky objects. Today, it stands as one of the most iconic galaxies in the night sky.
If you want the full image, you can download the 725 MB file from the project’s site. (via petapixel)

While reading this article about the structure of complex knots, I ran across this diagram drawn by scientist Peter Guthrie Tait in 1885 for a paper called On Knots Part III. It’s one of two figures that together show all of the possible variations of knots with 10 crossings. I think the color plus the small multiples activated the Tufte array in my brain; anyway, I love this diagram. (via damn interesting)
(I tried for the better part of an hour to track down a high-resolution copy of Tait’s paper to no avail. There are various contenders, but nothing that includes high-res scans of both knottiness diagrams. I’m curious about this archive of the original paper but not $41 curious. If anyone has access through their institution and wants to send me a PDF, I’d love that. Update: I have a copy of the paper and will be posting updated images soon! Thank you, Michael!)
This is an animal called the leaf sheep:

It’s a species of slug that is partially solar-powered, like a plant. Leaf sheep are kleptoplastic organisms that steal chloroplasts from algae, store them in their bodies, and then can rely on photosynthesis for their energy needs:
The Costasiella sea slug not only looks like a succulent—it acts like one, too. One of the few animals able to photosynthesize, this tiny invertebrate (also known as the leaf slug or leaf sheep) acquires chloroplasts by munching on Avrainvillea, a paddle-shaped seaweed with a velvety texture. It then stores those chloroplasts in its own body, which enables the slug to soak up sunlight and transform it into energy—a process that also gives the mollusk its green color.
The chloroplasts are stored in the horn-shaped structures called cerata located on the slugs’ backs. Cerata evolved to increase the surface area of these animals for use in respiration and surface area is very helpful if you run on solar panels.
And they’re also cute as a button! I mean, look at these things:

I’d vaguely heard of Project Plowshare but good god, what a ridiculous and dangerous waste of time and money.
At the height of the Cold War, nuclear weapons were seen not only as devices of destruction, but also as tools for progress. Project Plowshare was a bold attempt to use atomic explosions for more practical purposes: from digging canals and creating harbors to reshaping entire landscapes. This project was designed to push the limits of what seemed possible, but instead turned into an environmental disaster.
This reminds me of that episode of the Simpsons when Homer buys a gun and uses it around the house for everything, like changing the TV channel and opening beer cans. If the only tool you have is a hammer…
This is so cool: in the early 1900s, a mechanical engineer named Louis Brennan invented a self-balancing train that ran on a single track. This video demonstrates how the train worked using a clever system of gyroscopes.
This is the Brennan Monorail, a train from the early 1900s that seemed to defy the laws of physics. Not only did it keep itself perfectly balanced on a single rail, but it mysteriously leaned into corners without any driver input.
It’s kind of incredible how well Brennan’s system worked. It’s ingenious. (via messy nessy)
Bill Hammack, aka The Engineer Guy, is an amazing engineering educator and in this video he explains how duct tape is designed to simultaneously do three things well: “a) adhere with light pressure, b) stay in place, yet c) be removable”.
Controlling the stickiness of tape is of utmost importance. In fact, a key element of engineering tape is controlling its stickiness — and only by doing that can tape be wound into a useful roll. If the tape sticks too tightly to itself, we could not use it.
Gotta be honest: I was not expecting Silly Putty to make a relevant guest appearance during his explanation. And I love the ramp & ball test for tape stickiness near the end…a very elegant and simple bit of engineering:
Pressure sensitive tape predates much of the most elementary molecular understanding of adhesion; tape has been mass produced since the early twentieth century. That engineers developed and refined tape without this knowledge is no surprise — recall that the purpose of the engineering method is to solve problems before we have full scientific knowledge.
I went into this video not knowing anything about how a mid-19th century sunshine recorder might work and was genuinely delighted by the reveal. If you’d like to be similarly surprised, stop reading now and just watch the video.
…
…
The sunshine recorder was invented in 1853 for measuring the duration of bright sunshine over a day. The contraption consists of a solid glass ball that acts as a lens, which focuses the light of the Sun onto a paper recording card, burning marks into it. As the Sun moves across the sky, the focus point moves across the recording card, burning a line into it. If it’s super sunny out, the focused beam burns right through the card. So simple! So clever! And so straightforwardly physical — here’s what a daily sunshine record looks like:


(via robert stephens)
NASA has made available more than a dozen mobile wallpapers of photos taken during the Artemis II mission for free download. Basic Apple Guy has made some wallpapers of his own (that are slightly larger than NASA’s and better for iPhones). I have also made a few of my own: Earth Rising Over the Moon With the Orion Capsule in the Foreground, A Sliver of Earth Over the Moon, and Kubrickian Earth.
Here are a few of my favorites:



Interstitial tip: if you’re using an iPhone with iOS 26, tap the Spatial Scene button when you’re editing your wallpaper and the phone will turn any of these images into a 3D-ish scene that moves when you move your phone. Works best with images containing multiple objects (like the Earthrises). Makes you feel a little bit more like you’re there. (This is also an amazing setup.)






These are all real photos, cropped from the originals shared by NASA on Flickr and their website.
I also went back and looked at some of the images from the Artemis I mission, which sent an Orion capsule around the Moon without a human crew. Here are a few wallpapers made from photos from that mission: Earth Moon Capsule, Lens Flare Trio, and Lunar Surface.



Again, these three are from the Artemis I mission in late 2022. The first one works especially well with the Spatial Scene mode on iOS 26.

The commander of NASA’s Artemis II mission to the Moon, Reid Wiseman, took this photo of the Earth as the spacecraft speeds away our planet.
There are two auroras (top right and bottom left) and zodiacal light (bottom right) is visible as the Earth eclipses the Sun.
That is so cool. Worth clicking through to see the high-resolution image.

I love this planet & stars chart from XKCD because it’s technically correct but also completely useless.

During the recent annular solar eclipse on February 17, the ESA’s PROBA-2 satellite captured this great shot of the Moon passing in front of the Sun. Cue up the Johnny Cash.
Physicist Sean Carroll leads off this video with this line:
I like to say that Einstein is, if anything, underrated as a physicist, which is hard to imagine given how highly he is rated.
And then leads us through a history of modern physics and quantum mechanics that, Einstein and Newton aside, is much more collaborative than you often hear about.
This idea that there are many people contributing and many different parts of the pieces need to put together is actually much more characteristic of how physics is usually done than the single person inventing everything all by themselves.
Sleeping cleans your brain. Research suggests that zoning out, daydreaming, and being bored can perform a similar function without the need for deep sleep. So put down that phone occasionally and let your brain chill for a bit.

A recent paper in Nature details what scientists found at the Huayuan biota:
Here we report the Huayuan biota — a lower Cambrian (Stage 4, approximately 512 million years ago) BST Lagerstätte from an outer shelf, deep-water setting of the Yangtze Block in Hunan, South China. The Huayuan biota yields remarkable taxonomic richness, comprising 153 animal species of 16 phylum-level clades dominated by arthropods, poriferans and cnidarians, among which 59% of species are new. The biota is comprised overwhelmingly of soft-bodied forms that include preserved cellular tissues.
They have identified more than 50,000 individual fossil specimens that existed during what’s referred to as the Cambrian explosion, “when a sudden radiation of complex life occurred and practically all major animal phyla started appearing in the fossil record”. The fossils at the site are unusually intact:
Not only is this ecosystem notably diverse, but the fossils have remained unusually intact in the ancient mudstone, allowing for the preservation of soft tissues like tentacles, guts, and a nearly-complete nervous system found in one arthropod.
I’ve been interested in this period in paleontology since reading Stephen Jay Gould’s Wonderful Life: The Burgess Shale and the Nature of History in college. The Burgess Shale was a significant discovery that shed much light on the Cambrian explosion and surprisingly, paleontologists found fossils that appeared in both places.
The Burgess Shale animals date to about 508 million years ago, further removed from the Sinsk event than the Huayuan biota. Despite the vast distance separating the two sites, fossils of several of the same animals were found in the two locations.
“It surprised us when we found the Huayuan biota shared various animals with the Burgess Shale, including the arthropods Helmetia and Surusicaris that were previously only known from the Burgess Shale,” Zeng said.
“As larval stages are common in extant marine invertebrates, the best explanation of these shared taxa shall be that the larvae of early animals were capable of spreading by ocean currents since the early days of animals in the Cambrian,” Zeng said.
For those looking for more info on this discovery and its significance, paleontologist Dr. Joe Botting’s video on the Huayuan biota, which he calls “a stunning new Burgess Shale-type fauna”, might be a good place to start.
Bees use polarized sunlight scattered by the atmosphere in order to navigate; they always know where the sun is, even if it’s cloudy or behind a mountain. Then they waggle dance to inform their hive-mates about food source locations.
So if a bee wants to fly straight towards the sun, it waggles straight up the hive. If the food is 30° away from that polarization line, it waggles 30° away from vertical. If the food is directly away from the sun, it waggles downward.
And the distance they should fly is encoded on how long the waggle lasts. It depends on the species of bee, but a waggle of about 1 second means about a kilometer away. So a 45° waggle for about 0.6 seconds means fly at 45° angles from the sun polarization line for about 600 meters.
The bee repeats this waggle dance over and over. And the more excited the dance, the better the food source. And if other bees verify it and perform the same dance, the signal gets amplified until the whole hive knows where to go.
As shown in this video, it’s possible to construct an optical compass using polarized filters in order to wayfind like the bees. Pretty cool! (via damn interesting)
Nature magazine has chosen its favorite science images of the year. I’ve featured a few of these on the site already — Skydiving the Sun, red sprites in the New Zealand sky — so I picked a couple of other favorites to share:


The first was taken by Francisco Negroni of the Villarrica volcano in Chile (check out his site for more amazing photos of volcanos & lightning). The second is by 13-year-old Grayson Bell of two green frogs fighting; Bell named his photo “Baptism of the Unwilling Convert”.
In a recent bombshell piece for the New Yorker (archive), Rachel Aviv explored the personal journals of the celebrated neurologist and writer Oliver Sacks. What she found was shocking: he had fabricated and embellished some of his most well-known work — like Awakenings and The Man Who Mistook His Wife for a Hat. Sacks himself referred to his “lies” and “falsification” in journal entries.
But, in his journal, Sacks wrote that “a sense of hideous criminality remains (psychologically) attached” to his work: he had given his patients “powers (starting with powers of speech) which they do not have.” Some details, he recognized, were “pure fabrications.” He tried to reassure himself that the exaggerations did not come from a shallow place, such as a desire for fame or attention. “The impulse is both ‘purer’ — and deeper,” he wrote. “It is not merely or wholly a projection — nor (as I have sometimes, ingeniously-disingenuously, maintained) a mere ‘sensitization’ of what I know so well in myself. But (if you will) a sort of autobiography.” He called it “symbolic ‘exo-graphy.’”
Sacks had “misstepped in this regard, many many times, in ‘Awakenings,’” he wrote in another journal entry, describing it as a “source of severe, long-lasting, self-recrimination.”
The author Maria Konnikova discovered Sacks’ work in high school — “it blew my mind”, she writes. After the Aviv piece was published, Konnikova wrote a post about Sacks: The man who mistook his imagination for the truth.
When Joseph Mitchell invents a fishmonger, nobody gets hurt. It’s not journalism. It’s not nonfiction. But it’s not life or death. When Jonah Lehrer invents a quote from Bob Dylan, you can call him a narcissistic idiot for thinking he can get away with fabulizing a living legend whose every word has been studied. It’s not journalism. It’s not nonfiction. But, again, it’s not the end of the world. When Oliver Sacks invents an ability that does not exist or crafts a portrait of his own creation, he is hampering medical progress and tampering with the ethics of his profession. Not all journalistic malfeasance is created equal. There are plenty of shades of grey. But making up medical details is not in the gray zone. It’s malpractice.

From Domain of Science, the Fascinating Map of Fungi.
The zombie ant fungus, Ophiocordyceps unilateralis, infects ants by piercing the exoskeleton with enzymes and spreads fungal cells throughout the body. It then secretes special neurological compounds that hijack the ant’s central nervous system, forcing it to climb high into a tree and lock its mandibles onto a leaf with a death grip. This makes a nice stable platform for the fungus to grow a fruiting body to disperse spores in a large area to infect more hosts.
And here’s a video explanation of everything on the map.
See also this Classification of Plants & Fungi poster and its corresponding video explanation.
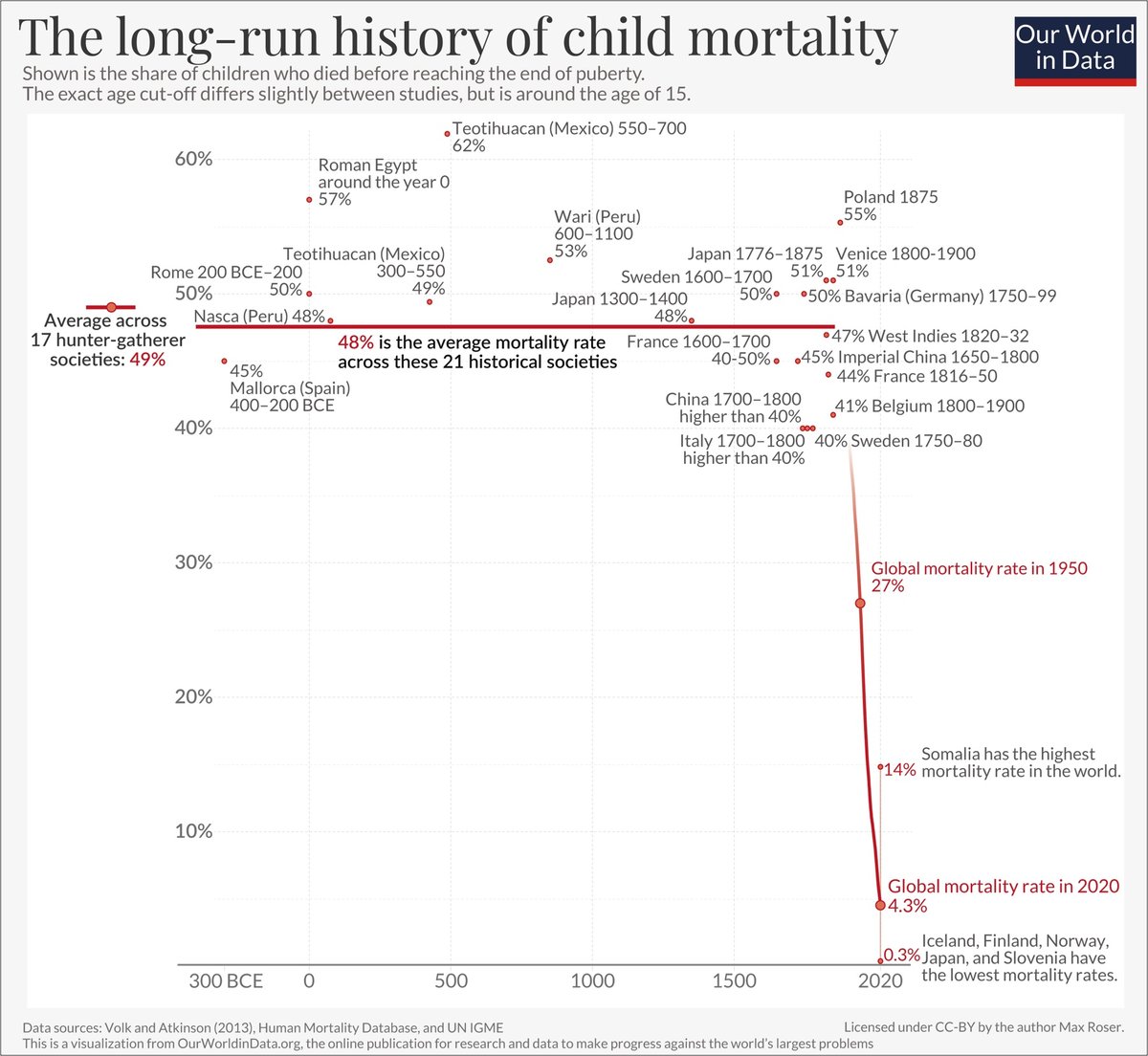
For most of human history, around 50% of children used to die before they reached the end of puberty. In 2020, that number is 4.3%. It’s 0.3% in countries like Japan & Norway.
This dramatic decline has resulted from better nutrition, clean water, sanitation, neonatal healthcare, vaccinations, medicines, and reductions in poverty, conflicts, and famine.
Before ~1800, almost every parent lost a child; now it’s such an uncommon experience that people have forgotten and want to ban vaccines.
In a letter to the Times of London, Dr. Michael Baum tells how a line in Arcadia by Tom Stoppard sparked an idea which resulted in adjuvant systemic chemotherapy, a therapy Baum helped pioneer which greatly increased the survivability of breast cancer.
Sir, In 1993 my wife and I went to see the first production of Arcadia by Tom Stoppard (obituary, Dec 1), and in the interval I experienced a Damascene conversion. As a clinical scientist I was trying to understand the enigma of the behaviour of breast cancer, the assumption being that it grew in a linear trajectory spitting off metastases on its way. In the first act of Arcadia, Thomasina asks her tutor, Septimus: “If there is an equation for a curve like a bell, there must be an equation for one like a bluebell, and if a bluebell, why not a rose?” With that Stoppard explains chaos theory, which better explains the behaviour of breast cancer. At the point of diagnosis, the cancer must have already scattered cancer cells into the circulation that nest latent in distant organs. The consequence of that hypothesis was the birth of “adjuvant systemic chemotherapy”, and rapidly we saw a striking fall of the curve that illustrated patients’ survival.
Stoppard never learnt how many lives he saved by writing Arcadia.
Michael Baum
Professor emeritus of surgery; visiting professor of medical humanities, UCL
Certainly drives home the value of a robust and diverse culture of humanities in contradiction to the current backlash. (via @harrywallop.co.uk)

We’ve talked before about how some people can picture things in their heads quite vividly and others can’t at all. The latter group has a condition called aphantasia.
As soon as I close my eyes, what I see are not everyday objects, animals, and vehicles, but the dark underside of my eyelids. I can’t willingly form the faintest of images in my mind.
Larissa MacFarquhar wrote a fascinating article about aphantasia (and its opposite, hyperphantasia) for the New Yorker: Some People Can’t See Mental Images. The Consequences Are Profound.
Naturally, aphantasics usually had a very different experience of reading. Like most people, as they became absorbed, they stopped noticing the visual qualities of the words on the page, and, because their eyes were fully employed in reading, they also stopped noticing the visual world around them. But, because the words prompted no mental images, it was almost as if reading bypassed the visual world altogether and tunnelled directly into their minds.
Aphantasics might skip over descriptive passages in books — since description aroused no images in their minds, they found it dull — or, because of such passages, avoid fiction altogether. Some aphantasics found the movie versions of novels more compelling, since these supplied the pictures that they were unable to imagine. Of course, for people who did have imagery, seeing a book character in a movie was often unsettling — because they already had a sharp mental image of the character which didn’t look like the actor, or because their image was vague but just particular enough that the actor looked wrong, or because their image was barely there at all and the physical solidity of the actor conflicted with that amorphousness.
And also:
When aphantasics recovered from bereavement, or breakups, or trauma, more quickly than others, they worried that they were overly detached or emotionally deficient. When they didn’t see people regularly, even family, they tended not to think about them.
M.L.: “I do not miss people when they are not there. My children and grandchildren are dear to me, in a muffled way. I am fiercely protective of them but am not bothered if they don’t visit or call. … I think that leaves them feeling as if I don’t love them at all. I do, but only when they are with me, when they go away they really cease to exist, except as a ‘story.’”
The bits about hyperphantasia are just as interesting:
Hyperphantasia often seemed to function as an emotional amplifier in mental illness—heightening hypomania, worsening depression, causing intrusive traumatic imagery in P.T.S.D. to be more realistic and disturbing. Reshanne Reeder, a neuroscientist at the University of Liverpool, began interviewing hyperphantasics in 2021 and found that many of them had a fantasy world that they could enter at will. But they were also prone to what she called maladaptive daydreaming. They might become so absorbed while on a walk that they would wander, not noticing their surroundings, and get lost. It was difficult for them to control their imaginations: once they pictured something, it was hard to get rid of it. It was so easy for hyperphantasics to imagine scenes as lifelike as reality that they could later become unsure what had actually happened and what had not.
“I can imagine my hand burning, to the point where it’s painful. I’ve always been curious — if they put me in an fMRI, would that show up? That’s one of the biggest problems in my life: when I feel something, is it real?”
One hyperphantasic told a researcher that he had more than once walked into a wall because he had pictured a doorway.
The more I read about this, the more I think that for those at either end of the phantasic scale, their inability (or extreme ability) to see things in their minds is a major component of what we think of as personality. Even just thinking about myself, there are all sorts of behaviors and traits I can connect to not being able to visualize things in my head that clearly. In some ways, it might be one of the most me things about me. (thx, willy)
Two reasons why XKCD’s What If? series is so compelling:
- Even when an answer seems straightforward, the devil is in the details.
- And with respect to the details, Munroe does his due diligence.
In this case, the answer to “what’s the longest possible sunset you can experience while driving, assuming you’re obeying the speed limit and driving on paved roads?” was fairly surprising and exact and the explanation delightful.
Btw, the ending of the video is a callback to an early XKCD comic about angular momentum.
Stress in pre-modern times was a “biological superpower” that helped humans hunt for food and survive in harsh environments and situations. But our bodies can’t easily tell the difference between the stress of encountering a lion in the jungle and a worrying email from your boss.
Our world has changed so quickly and profoundly that our biology couldn’t keep up. Stress is still the same it was fifty thousand years ago: Sense a stressor. React immediately and with full force. Prioritize present moment survival, make sacrifices if necessary.
That works well when you have to jump out of the way of a car. But most stressors we encounter nowadays are abstract, acute and more numerous, often intangible, persist for much longer and usually don’t even require physical action. The tigers of the past are now angry emails, deadlines, online dating, rush hour traffic or doom scrolling the news and social media.
Note: Watching this video might actually stress you out, at least until you get to the solutions part of it.
Caveat: In places with a lot of economic insecurity & few social safety nets, like the US, the solutions presented by this video may not be super helpful. Slowing down, disconnecting, and taking time for mindfulness can be difficult under the best of conditions and nearly impossible if you’re working two jobs as a single mother to just make ends meet.
From MinuteEarth, a quick tour of all the different kinds of cats in the world, extinct, wild, and domesticated, and how they are related to each other. Some interesting facts I learned:
- The saber-toothed tiger was the largest cat to ever live and researchers now believe it had a short tail rather than a long one.
- There was an American cheetah. It was bigger than the cheetah we know today and “almost as fast”. It went extinct around the time humans showed up in North America.
- Leopards and snow leopards aren’t actually that closely related.
- Domestic cats are mostly descended from wildcats (not to be confused with cats who are wild — wildcat refers to two specific species, the European wildcat (Felis silvestris) and the African wildcat (Felis lybica)).
See also All the Dogs, Explained: “Standing on his hind legs, [the tallest ever Great Dane] was taller than Shaq.”
Operation Space Station is a two-part PBS documentary series on the International Space Station. Here’s a very short teaser trailer:
A synopsis:
The size of a football field, the International Space Station hurtles around Earth at 17,000 mph, shielding its astronauts from the most hostile environment humans have ever endured. After 25 years of continuous human presence in space, astronauts and Mission Control insiders reveal the most terrifying moments aboard this remarkable orbiting laboratory, where a single mistake could prove fatal. From ammonia leaks, meteor strikes, and docking disasters, to spacewalk horrors, potentially lethal showers of space junk, and the moment the entire ISS backflipped out of control, follow life-or-death dramas unfolding 250 miles above our planet — and the human ingenuity and teamwork that save the day.
(via installer)
A few years ago, a researcher looked at every surviving print of Hokusai’s The Great Wave off Kanagawa that she could find (113 in all) and, using differences caused by “woodblock wear”, developed a system for determining if a particular print was made early in the life of the woodblocks used, late, or somewhere in-between.
Did you know there are 113 identified copies of Hokusai’s The Great Wave. I know the title says 111, but scientist Capucine Korenberg found another 2 after completing her research. What research was that? Finding every print of The Great Wave around the world and then sequencing them, to find out when they were created during the life cycle of the woodblocks they were printed from.
This involved painstakingly documenting visible signs of wear to the keyblock that made the Great Wave, and tracking these visible changes as the keyblock continued to be used (fun fact; scholars estimate there were likely as many as 8000 prints of The Great Wave originally in circulation).
See also The Evolution of Hokusai’s Great Wave.
The latest video from Kurzgesagt imagines a scenario in which an advanced civilization called the Noxans can potentially survive the heat death of the universe.
With five hours of the full energy emitted by the Sun, we could power present day humanity for about 10 billion years.
So the Noxans harvest the last stars and build a gigantic complex of batteries around their home star. In principle, this energy could keep them alive for a few hundred trillion years, a long time but not even close to forever.
So now the hard part of the plan begins. The Noxans need to change the nature of life itself.
Steve Mould is always informative and entertaining, so I started watching his video on building the world’s tallest siphon, nodding along to what I thought was the reasonable conclusion. And then the video kicked into another gear — because with science, the simple solution is not always the whole story when extreme conditions are in play. (via the kid should see this)
In the most recent episode of Howtown, Joss Fong explains how above-ground nuclear testing in the 50s and 60s left a signature in all life on Earth that can be used as a forensic tool for catching art forgers, shady ivory dealers, and even fraudulent wine sellers/cellars.
In the 1950s and early 1960s, the United States and the Soviet Union (with contributions from the UK and France) conducted a series of above-ground nuclear tests that led to an increase in the radioactive carbon-14 concentration in the atmosphere. This global surge, known as the “bomb pulse” or the “bomb spike”, is one of the most distinctive chemical signatures of the Cold War. The radiocarbon spread worldwide, embedding into plants, animals, and humans.
Scientists later discovered that this bomb-pulse radiocarbon spike could be used as a precise dating tool. Bomb-pulse dating allows researchers to determine whether biological material formed before or after nuclear testing. This method has been applied to forensic science, medical research, and environmental monitoring. It has been used to identify forgeries in artwork, measure human cell turnover, and estimate the lifespan of Greenland sharks.
One of the most important applications has been in tracking the illegal ivory trade. Elephant tusks absorb atmospheric carbon while the animal is alive. By analyzing the carbon-14 content of ivory artifacts or raw ivory, investigators can determine whether the material comes from a legally antique source or from a recently killed elephant.
This intersection of nuclear history, atmospheric science, and conservation biology demonstrates how Cold War nuclear fallout became a forensic tool for fighting elephant poaching and wildlife trafficking. More broadly, it demonstrates the creativity and resourcefulness of scientific researchers, who find ingenious uses for datasets of unlikely origin.
I ran across this delightful account that explores and explains everyday scientific questions through maddeningly catchy songs. Like why a cast saw cuts through plaster but spares your skin:
How working principle of an electric kettle is another banger:
My gateway into this account was why are steel coils placed upright when trucks are hauling them:
These will get stuck in your head. Available on YouTube and TikTok (e.g. how is a football made).
Older posts































Socials & More